Adverse Effects of Transfusion
Blood transfusion is a life-saving procedure in an appropriate setting and there are no side-effects in the majority of cases. However, it is a potentially harmful procedure and every recipient of transfusion is at risk of an adverse reaction. It should be prescribed only if there is a definite clinical indication. This is because even with best possible blood banking standards, transmission of infections or other complications can occur.
Adverse effects of transfusion are listed in Table 1196.1.
| Immediate | Delayed |
| 1. Acute hemolytic transfusion reaction | 1. Delayed hemolytic transfusion reaction |
| 2. Febrile non-hemolytic transfusion reaction | 2. Transmission of infections |
| 3. Allergic reactions | 3. Iron overload |
| 4. Anaphylactic reactions | 4. Graft vs. host disease |
| 5. Transfusion-associated lung injury | 5. Post-transfusion purpura |
| 6. Volume overload | - |
| 7. Bacterial contamination of the donor unit | - |
Main causes of transfusion-related deaths are:
- Immediate acute hemolytic transfusion reaction (ABO incompatibility)
- Pulmonary edema and congestive heart failure (circulatory overload)
- Bacterial contamination of blood unit
- Transfusion of physically damaged red cells (e.g. by heat, cold)
- Transfusion-associated graft vs. host disease
ACUTE HEMOLYTIC TRANSFUSION REACTION
This is a medical emergency and results from intravascular destruction of donor red cells by antibodies in the recipient. It results from transfusion of ABO-mismatched blood to the recipient due most commonly to a clerical error. Most severe reaction occurs if group A blood is transfused to a group O recipient.
Pathophysiology consists of antigen-antibody reaction that leads to complement activation and intravascular hemolysis. This causes hypotension, shock, acute renal failure, and disseminated intravascular coagulation (Figure 1196.1). Signs and symptoms (that appear within minutes of starting transfusion) include fever, pain at the infusion site, loin pain, tachycardia, hemoglobinuria, and hypotension. In anesthetized patients, bleeding and hypotension are the only indications.
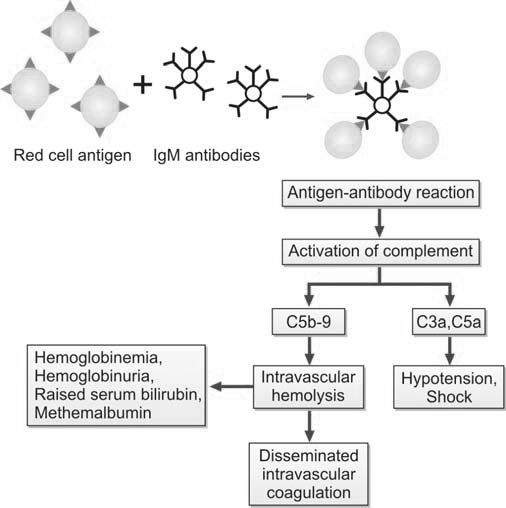
Laboratory features are:
- Hemoglobinemia (pink coloration of plasma after centrifugation of post-transfusion sample)
- Positive direct antiglobulin test
- Hemoglobinuria
- Schistocytes (fragmented red cells) and spherocytes on blood smear
- Elevated indirect serum bilirubin
FEBRILE NON-HEMOLYTIC TRANSFUSION REACTION
This is the most common transfusion reaction. It occurs in about 1% of all transfusions and is defined as an unexplained rise of temperature of at least 1°C during or shortly after transfusion. It is caused by the release of pyrogenic cytokines from white cells (during storage of blood unit or following transfusion due to the reaction of alloantibodies with white cells of donor). This reaction is common in multiply-transfused patients. Signs and symptoms include fever, chills, and tachycardia. Diagnosis depends on the exclusion of other causes of febrile transfusion reaction.
Transfusion reactions presenting with fever are shown in Figure 1196.2.
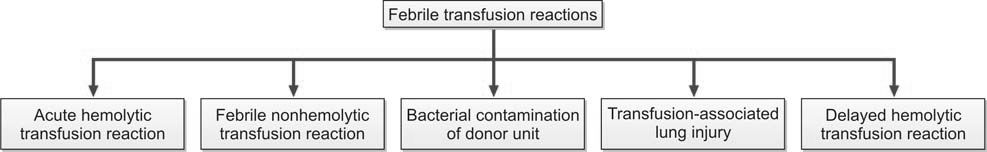
BACTERIAL CONTAMINATION OF DONOR UNIT
Transfusion of an infected blood product is more common with platelet concentrates since platelets are stored at a higher temperature (20-24°C) that promotes multiplication of contaminating bacteria. Organisms depend on the nature of the blood product. Platelets are usually contaminated with gram-positive cocci, while red cells are contaminated with Yersinia enterocolitica, Escherichia coli, or Pseudomonas species. Signs and symptoms include high-grade fever with rigors, hypotension, and shock. Laboratory studies include inspection of blood bag for discoloration and Gram staining and culture of blood from the blood bag and from the recipient. Direct antiglobulin test is negative.
TRANSFUSION-ASSOCIATED LUNG INJURY
This is an acute respiratory disorder that manifests with fever, chills, dyspnea, and dry cough. X-ray shows diffuse pulmonary infiltrates. One probable mechanism is reaction of anti-HLA or anti-neutrophil antibodies in donor blood with leukocytes of the recipient leading to the formation of leukocyte aggregates; these aggregates deposit in pulmonary vasculature and cause increased vascular permeability and pulmonary edema.
DELAYED HEMOLYTIC TRANSFUSION REACTION
This is a hemolytic transfusion reaction occurring several days or weeks after transfusion. This occurs in individuals who have been sensitized to a red cell antigen by a previous transfusion or pregnancy so that the antibody is present in a low titer. On re-exposure, there is a secondary IgG immune response and mainly extravascular hemolysis. This reaction is typically associated with Kidd antibodies.
Signs and symptoms include fever, mild jaundice, and mild anemia. Laboratory features include raised indirect serum bilirubin, spherocytes on blood smear, anemia, and positive direct antiglobulin test. Acute and delayed hemolytic transfusion reactions are compared in Table 1196.2.
| Parameter | Acute | Delayed |
| 1. Type of antibody | Anti-ABO | Anti-Kidd |
| 2. Nature of antibody | Naturally-occurring | Immune |
| 3. Time of appearance of clinical features after transfusion | Within minutes | After several days or weeks |
| 4. Site of hemolysis | Intravascular | Extravascular |
| 5. Clinical features | Fever, chills, back pain, acute renal failure, DIC | Fever, mild jaundice, anemia |
ANAPHYLACTIC REACTION
This rare reaction occurs in IgA-deficient recipients in whom anti-IgA antibodies react with IgA in donor plasma, leading to activation of complement and formation of anaphylatoxins (C3a and C5a). Signs and symptoms include the development of acute hypotension, shock, and dyspnoea after transfusion of a few drops of blood.
ALLERGIC REACTION
This results from type I hypersensitivity reaction to some donor plasma proteins. It is the second most frequently reported transfusion reaction. Signs and symptoms include mild urticaria, rash, and pruritus.
VOLUME OVERLOAD
This occurs if transfusion rate is too rapid, or excessive, or if cardiac or renal impairment is present. It causes cardiac failure and lung edema.
IRON OVERLOAD
Each unit of blood contains 200 mg of iron. Patients receiving regular transfusion therapy such as those with thalassemia develop manifestations of parenchymal damage due to iron accumulation.
TRANSMISSION OF INFECTIONS
Organisms transmissible by transfusion are listed in Table 1197.1 (See article: Screening Tests for Infections Transmissible by Transfusion).
- Hepatitis A virus: Hepatitis A is rarely transmitted by transfusion, as the duration of viremia is short. Donors with hepatitis A or who are in close contact with a hepatitis A are deferred for 1 year.
- Hepatitis B virus: In India, prevalence of hepatitis B virus is 1.5 to 4%, and there are 43 million carriers. Hepatitis B virus, a DNA virus, can be transmitted by both cellular and plasma components. Incubation period is 2-6 months. All blood donations are tested for HBsAg by a sensitive method that has greatly reduced the risk of transmission. During early period of infection, HBsAg may be undetectable; during this window period, antibodies to the hepatitis B core antigen (anti-HBc) may be the only evidence of disease. HBsAg-positive donors are permanently excluded from donations. Liver diseases caused by hepatitis B virus include: subclinical hepatitis, acute icteric hepatitis, fulminant hepatitis (massive hepatic necrosis), chronic hepatitis, cirrhosis, and hepatocellular carcinoma.
- Hepatitis C virus: In India, prevalence of hepatitis C virus is reported to be 1.66% and there are 15 million carriers. This RNA virus is the most common cause of transfusion-transmitted hepatitis. It is transmitted by both cellular and plasma components. Incubation period is about 8 weeks. Persistent infection is the rule. Chronic hepatitis is very common (usually mild). Cirrhosis occurs in a minority of patients, and hepatocellular carcinoma occurs in about 10% with cirrhosis. The test used for donor screening is anti-HCV antibody test. From infection till the appearance of anti-HCV positivity (70-80 days), HCV RNA can be detected by PCR testing.
- Human immunodeficiency virus (HIV): In India, adult prevalence is 0.7%. Two genetically different but closely related viruses are recognized: HIV-1 and HIV-2. Both are RNA retroviruses. Natural history of HIV infection consists of (i) acute, self-limited, “flulike” illness occurring 3-6 weeks after infection, (ii) chronic phase lasting for several years that may be asymptomatic or associated with persistent lymphadenopathy, and (iii) final, full-blown phase with opportunistic infections and malignancies. HIV can be transmitted by both cellular and plasma components. The test used for detection of infection is anti-HIV-1/2 antibodies by enzyme immunoassay. To reduce the window period from infection to appearance of antibodies from about 22 days to 10 days, nucleic acid testing (NAT) for HIV RNA is recommended.
- Treponema pallidum: Trasfusion-transmission of syphilis is rare since T. pallidum does not survive in refrigerated storage and is inactivated at 4°C after 4 days; however, fresh blood and platelet concentrates can transmit the organism. The main value of screening test is as a marker of high-risk behavior.
- Malaria parasites: Malaria parasites are readily transmitted by transfusion. In endemic areas, it is not practical to reject all potential donors with history of malaria in the past. In endemic areas, the only safe prevention is administration of preventive antimalarial drugs to all recipients of transfusion.
COMPLICATIONS ASSOCIATED WITH MASSIVE TRANSFUSION
Massive transfusion refers to transfusion of stored blood equivalent to patient’s blood volume in 24 hours. Morbidity and mortality is due to rapid blood loss coupled with transfusion of stored blood.
Storage of blood is associated with loss of 2,3-diphosphoglycerate, lowering of pH, loss of ATP, loss of platelet function, and depletion of coagulation factors. Microaggregates composed of leukocytes and platelets form gradually in stored blood. Rapid transfusion of large volumes of stored blood leads to:
- Dilution of platelets and coagulation factors
- Hyperkalemia (due to release of potassium from stored red cells)
- Hypocalcemia (due to binding of calcium by citrate)
- Hypothermia (due to rapid infusion of large amount of cold blood)
- Adult respiratory distress syndrome due to migration of microaggregates to lungs.
RECOGNITION AND INVESTIGATION OF A TRANSFUSION REACTION
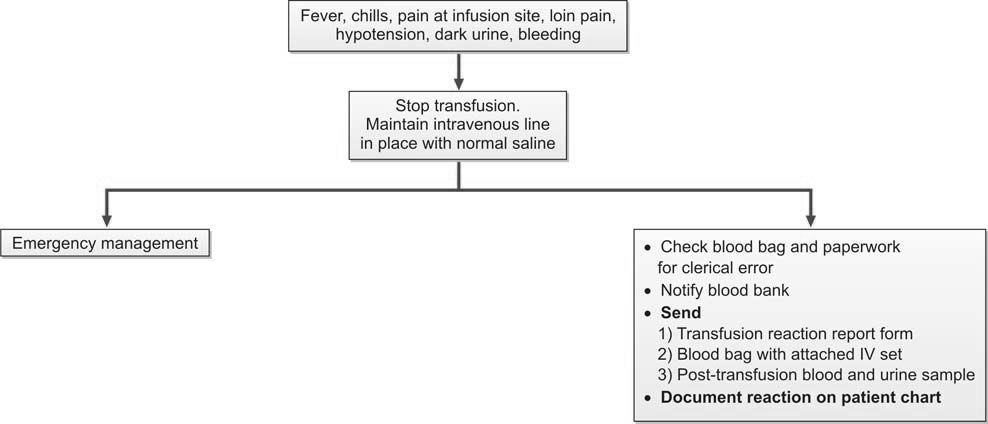
All reactions following blood transfusion should be considered as hemolytic in nature and should be investigated accordingly (Figure 1196.3).
- Transfusion should be immediately stopped, leaving open intravenous line with normal saline.
- All paperwork and blood bag should be checked for clerical error. More than 90% of hemolytic transfusions result from a clerical error (i.e. a wrong unit of blood is given to the wrong recipient).
- Blood bank is informed immediately and the blood bag, administration set, and post-transfusion blood and urine samples should be sent to the blood bank.
- Evidence of hemolysis: Obtain a post-transfusion blood sample from the recipient, centrifuge, and observe for pink discoloration of overlying plasma (hemoglobinemia); this is the most rapid way of detecting intravascular hemolysis if pre-transfusion sample is normal. Similarly, visual examination of patient’s urine can be done for hemoglobinuria. Blood smear examination will show fragmented red cells and spherocytes. Indirect serum bilirubin is raised.
- Evidence of blood group incompatibility: Perform a direct antiglobulin test (DAT) on post- and pretransfusion blood samples. Positive DAT on posttransfusion sample (with negative test on pretransfusion sample) is indicative of an immunological hemolytic transfusion reaction. Blood group incompatibility will also be revealed on (i) repeat ABO grouping on recipient’s pre- and post-transfusion samples and on donor unit, and (ii) repeat crossmatching of donor blood against recipient’s pre- and post-transfusion samples.
- Investigations for detection of complications of hemolytic transfusion reaction:
• Tests for disseminated intravascular coagulation: Blood smear, coagulation screen, and test for fibrin degradation products
• Tests for acute renal failure: Blood urea, serum creatinine, and serum electrolytes - Bacteriological culture if the cause of the acute transfusion is still not clear.
References
- World Health Organization: Blood Transfusion Safety: The Clinical Use of Blood. Geneva: World Health Organization, 2002.
- Comment
- Posted by Dayyal Dg.
- Hemotology
- Hemotology Notes
- Article
- Blood Transfusion Reaction
- Blood Transfusion
- Massive Blood Transfusion Complications
- Jehovah Witness Blood Transfusion
- Blood Infusion
- Blood Transfusion Definition
- Blood Transfusion Reasons
- Blood Transfusion Meaning
- Blood Transfusion Procedure
- Complications of Blood Transfusion