How to Count Reticulocytes (Manual Method)
Learn manual reticulocyte count methods: supravital staining, Miller ocular disk technique, formulas (%, absolute, corrected, RPI), reference ranges, and clinical interpretation for anemia diagnosis and bone marrow assessment.
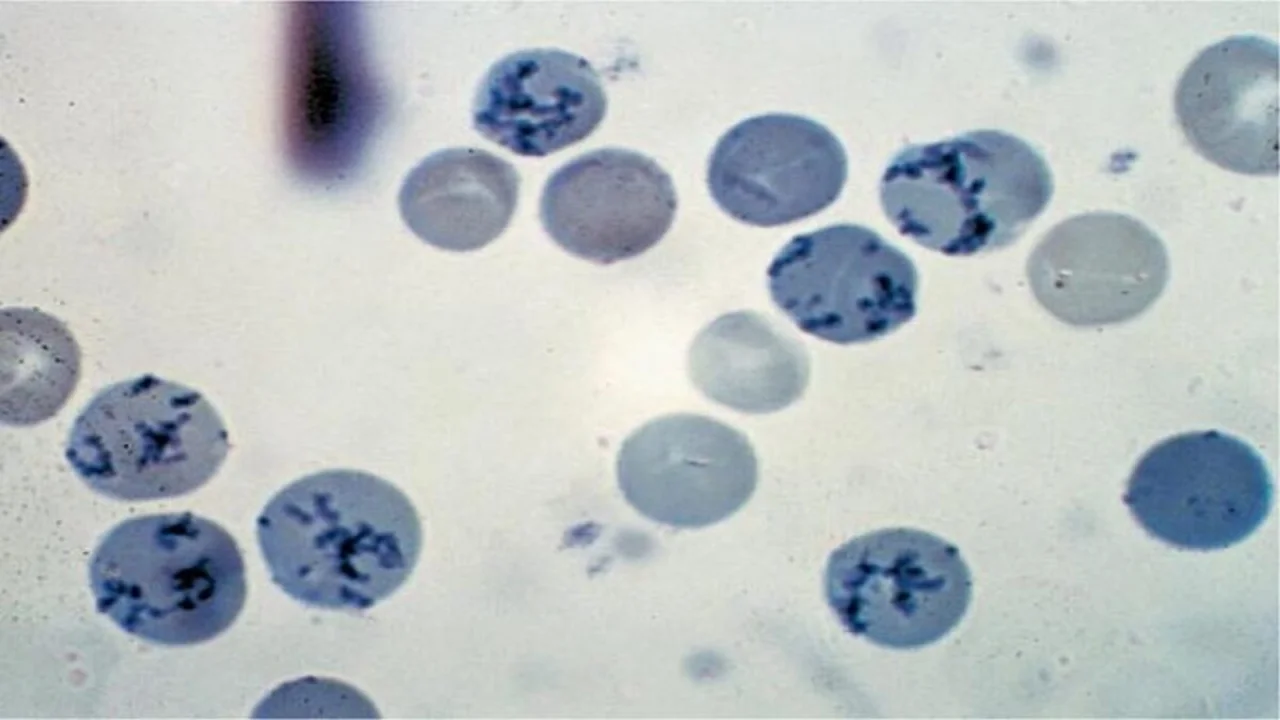
Reticulocytes are immature red blood cells (RBCs) released from bone marrow into the bloodstream, characterized by residual ribonucleic acid (RNA) and ribosomes. Identified via supravital staining (e.g., new methylene blue), they exhibit 2+ blue-stained RNA granules/filaments (per College of American Pathology criteria). These cells mature into RBCs within 1–2 days, and their count—a key marker of bone marrow activity—is typically measured manually in clinical laboratories.
Principle
Manual reticulocyte count is a laboratory technique based on the principle of supravital staining to detect residual ribosomal RNA in immature red blood cells (RBCs), quantifying bone marrow erythropoietic activity. EDTA-anticoagulated blood is incubated with a supravital dye (e.g., new methylene blue), which binds RNA, forming blue-stained granules or filaments. A blood smear is manually examined under a microscope, and reticulocytes are counted as a percentage of total RBCs. This method leverages RNA’s affinity for supravital dyes in unfixed, living cells, ensuring precise identification of immature RBCs for diagnosing anemia and assessing marrow function.
Reagent
- New Methylene Blue:
- New methylene blue: 1.0 gm
- Sodium citrate: 0.6 gm
- Sodium chloride: 0.7 gm
- Distilled water: 100 ml
- Brilliant Cresyl Blue:
- Brilliant cresyl blue: 1.0 gm
- Sodium citrate: 0.6 gm
- Sodium chloride: 0.7 gm
- Distilled water: 100 ml
Reagent should be kept stored in a refrigerator at 2-6°C and filtered before use.
Suitable alternatives to new methylene blue are brilliant cresyl blue and azure B.
Specimen
Capillary blood or EDTA anticoagulated venous blood can be used.
Procedure
- Mix 2-3 drops of filtered new methylene blue dye with an equal volume of blood in a 12×75 mm test tube.
- Incubate at room temperature or 37°C for 15 minutes.
- Prepare a thin smear, air-dry, and examine under an oil-immersion microscope; reticulocytes display ≥2 blue ribosomal RNA particles.
- Count 1000 RBCs using a Miller ocular disk (to minimize error) and calculate the percentage.
What is Miller ocular disk?
A Miller ocular disk is a specialized eyepiece grid used in hematology microscopy to improve accuracy during manual cell counting, particularly for reticulocytes. It features two squares: a smaller square (1/10th the area of the larger) for counting red blood cells (RBCs) and a larger square to track reticulocytes along its borders. This design minimizes counting errors by standardizing field movement and ensuring consistent cell enumeration.
Features & Use:
- Grid Ratio: 9:1 (large:small square) for simultaneous RBC and reticulocyte tracking.
- Error Reduction: Separates counting zones to prevent overlap confusion.
- Application: Critical in reticulocyte count procedures to assess bone marrow response.
Reporting the Result
1. Reticulocyte percentage
Reticulocyte percentage measures immature red blood cells (reticulocytes) as a proportion of total red blood cells (RBCs), reflecting bone marrow’s erythropoietic activity. Calculated as:
Reference Ranges
- Adults/Children: 0.5%–2.5%
- Newborns: Higher (2%–6%), gradually declining to adult levels by 2 weeks.
Clinical Relevance
- Elevated %: Indicates bone marrow response to anemia (e.g., hemolytic anemia, hemorrhage, recovery post-treatment).
- Low %: Suggests impaired RBC production (e.g., iron/B12 deficiency, aplastic anemia, bone marrow suppression).
- Interpretation: Adjusted via Reticulocyte Production Index (RPI) to account for anemia severity.
2. Absolute Reticulocyte Count
Absolute reticulocyte count (ARC) quantifies the actual number of immature red blood cells (reticulocytes) per microliter of blood, providing a direct measure of bone marrow’s erythropoietic output. Calculated as:
Normal Range
- 50,000–85,000 reticulocytes/µL (cmm).
Clinical Significance
- Anemia Evaluation: Distinguishes between bone marrow response (e.g., elevated ARC in hemolysis or hemorrhage) and inadequate production (e.g., low ARC in aplastic anemia or nutritional deficiencies).
- Superior to Percentage Alone: Adjusts for anemia severity (e.g., a “normal” reticulocyte % may still reflect low production in severe anemia).
- Monitoring: Tracks recovery during treatment (e.g., rising ARC after iron/B12 therapy).
3. Corrected Reticulocyte Count
Corrected reticulocyte count (CRC), also called the Reticulocyte Index, adjusts the reticulocyte percentage to account for anemia severity, providing a true measure of bone marrow’s response. Calculated as:
Interpretation
- CRC > 2%: Indicates adequate bone marrow response (e.g., hemolytic anemia, blood loss).
- CRC < 2%: Suggests inadequate erythropoiesis (e.g., iron deficiency, aplastic anemia, bone marrow failure).
Purpose
- Adjusts for Anemia: Prevents overestimation of reticulocyte production in anemic patients.
- Clinical Utility: Differentiates effective vs. ineffective marrow response in anemia workup.
4. Reticulocyte Maturation Production Index
Reticulocyte Maturation Production Index (RPI) quantifies bone marrow’s effective erythropoietic response by adjusting the corrected reticulocyte count for premature release and maturation time of reticulocytes in peripheral blood.
Calculation Factors & Interpretation
- Maturation Time: 1 day (Hct ≥40%), 1.5 days (Hct 30–40%), 2 days (Hct 20–30%), 2.5 days (Hct <20%).
- Interpretation:
- RPI ≥3: Robust marrow response (e.g., hemolytic anemia, acute blood loss).
- RPI <2: Inadequate production (e.g., iron deficiency, aplastic anemia).
Purpose
- Adjusts for Anemia Severity: Accounts for prolonged reticulocyte maturation in severe anemia.
- Clinical Utility: Distinguishes appropriate vs. inadequate bone marrow compensation.
Clinical Significances
- Reticulocytosis (Elevated Counts):
- Causes:
- Hemolytic Anemias (e.g., immune hemolysis, sickle cell disease, enzyme deficiencies).
- Acute blood loss or hemorrhage.
- Recovery post-treatment (e.g., iron/B12 supplementation).
- Physiologic increases (e.g., pregnancy, neonates).
- Significance: Indicates robust bone marrow response to RBC loss or destruction.
- Causes:
- Reticulocytopenia (Low Counts):
- Causes:
- Bone Marrow Suppression (e.g., aplastic anemia, chemotherapy, radiation).
- Nutritional Deficiencies (untreated iron/B12 deficiency).
- Infiltration (e.g., metastatic cancer, myelofibrosis).
- Significance: Suggests impaired RBC production or marrow dysfunction.
- Causes:
- Diagnostic Utility:
- Reticulocyte Production Index (RPI): Adjusts counts for anemia severity to differentiate true marrow response (e.g., hemolysis) from ineffective erythropoiesis (e.g., iron deficiency).
- Monitoring: Tracks recovery in treated anemias (e.g., rising reticulocytes after B12 therapy in pernicious anemia).
FAQs
How is reticulocyte count done?
How is reticulocyte count reported?
What does reticulocyte count indicate?
When is reticulocyte count increased?
When is reticulocyte count low?
Which stain is used for reticulocyte count?
Why is reticulocyte count low in iron deficiency anemia?
Why is reticulocyte count high in hemolytic anemia?
Why does reticulocyte count increase in thalassemia?
Why is reticulocyte count low in megaloblastic anemia?
The information on this page is peer reviewed by a qualified editorial review board member. Learn more about us and our editorial process.
Last reviewed on .
Article history
- Latest version
Reference(s)
- Bain, Barbara J.., et al. “Dacie and Lewis Practical Haematology.” 12th ed., Elsevier, 2017, isbn: 9780702066962. <https://www.sciencedirect.com/science/article/pii/B9780702066962099951>.
Cite this page:
- Posted by Dayyal Dungrela