CLASSIFICATION OF DIABETES MELLITUS
Diabetes mellitus (DM) is a metabolic group of disorders characterized by persistent hyperglycemia due to deficiency and/or diminished effectiveness of insulin. There are derangements of carbohydrate, protein, and fat metabolism due to failure of insulin action on target cells.
CLASSIFICATION OF DIABETES MELLITUS
According to American Diabetes Association (1997), DM is classified into following types:
- Type 1 (Absolute deficiency of insulin due to destruction of β cells of pancreas)
– Immune mediated
– Idiopathic - Type 2 (Insulin resistance along with relative deficiency of insulin secretion)
- Other specific types
- Gestational DM (onset or first recognition of glucose intolerance during pregnancy).
Type 1 Diabetes Mellitus
It accounts for 5-10% of all cases of DM. This was previously called as insulin-dependent DM or IDDM (because insulin therapy is essential to prevent ketosis), juvenile-onset DM (because it commonly presents during childhood or adolescence), brittle DM, or ketosis-prone DM. It is characterized by absolute deficiency of insulin secretion.
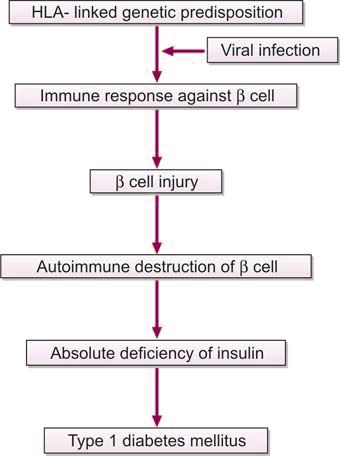
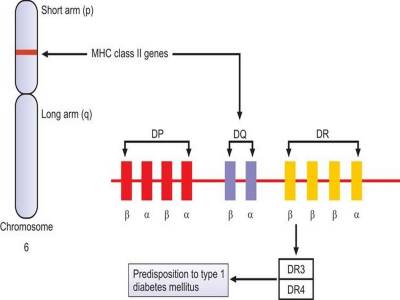
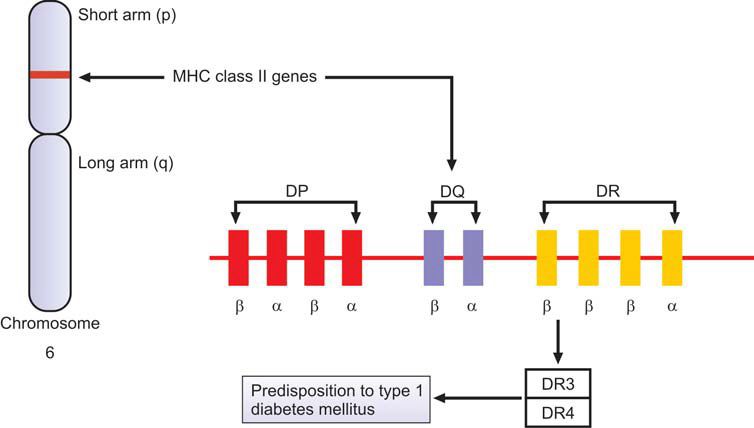
Cell-mediated autoimmune destruction of β cells of pancreas is responsible for majority of cases of type 1 DM (immune-mediated type 1 DM), leading to inability of pancreas to synthesize insulin. There is infiltration by cytotoxic CD8+ T lymphocytes in and around islets. It is thought that many cases follow a viral infection that has damaged the islet cells of pancreas (Figure 1191.1). Markers of immune destruction of β cells, which can be detected in peripheral blood, are islet cell antibodies, autoantibodies to insulin, autoantibodies to glutamic acid decarboxylase (GAD65), and autoantibodies to tyrosine phosphatases (IA-2 and IA-2b). The disease has strong association with HLA DR3 and HLA DR4 haplotypes (Figure 1191.2). This type occurs mainly in children and adolescents, but can occur at any age. These patients are also at risk of other autoimmune disorders like Graves’ disease, Hashimoto’s thyroiditis, vitiligo, Addison’s disease, pernicious anemia, etc.
Some cases of type 1 DM do not have any known etiologies or evidence of autoimmunity. These individuals are of Asian or African origin and their disease is strongly inherited. This form of type 1 DM is called as idiopathic DM.
Type 2 Diabetes Mellitus
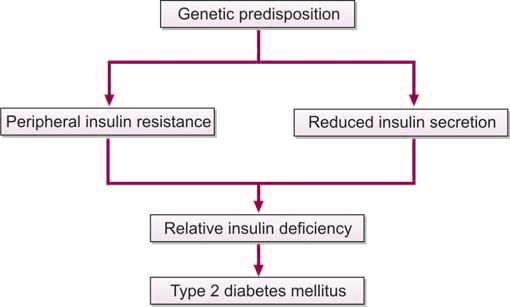
This is the most common form of DM comprising about 90-95% of all patients of DM. This was previously called as non-insulin-dependent DM (NIDDM), maturity-onset DM (because onset usually occurs during adult life), stable DM, or ketosis-resistant DM. It is characterized by insulin resistance along with relative deficiency of insulin secretion (i.e. inadequate insulin secretory response to overcome peripheral insulin resistance). (Figure 1191.3). Type 2 DM is not HLA-linked and there is no role of autoimmunity in its pathogenesis. It has a strong genetic predisposition. Type 2 DM occurs more frequently in individuals with positive family history (parents or siblings with DM), obesity (≥ 20% over ideal body weight or body mass index ≥ 25 kg/m2), hypertension (>140/90 mm Hg in adults), dyslipidemia, lack of physical activity, pre-diabetes (impaired fasting glucose or impaired glucose tolerance), and prior gestational DM.
Type 2 diabetes is more common in certain racial groups like South Asians and Africans. Rising trend of type 2 DM is due to increasing tendency towards obesity in urban populations coupled with high-calorie diet.
Differences between type 1 and type 2 Diabetes are listed in Table 1191.1.
| Parameter | Type 1 DM | Type 2 DM |
| 1. Previous names | Type I, IDDM, Juvenile-onset, Ketosis-prone, Brittle | Type II, NIDDM, maturity-onset, Ketosis-resistant, Stable |
| 2. % of all DM cases | 5-10% | 90-95% |
| 3. Age of onset | < 35 years | > 35 years |
| 4. Obesity | No (weight loss common) | Common |
| 5. Presentation | Acute; symptoms (classical) since few weeks | Insidious; symptoms since few months or years |
| 6. Genetic predisposition | Low | Strong |
| 7. Glucose intolerance | Marked | Mild |
| 8. Ketoacidosis | Common | Uncommon |
| 9. Hyperosmolar hyperglycemic state | Uncommon | Common |
| 10. Serum insulin | Undetectable | Normal or high |
| 11. Autoimmunity (Islet cell antibodies) | Majority of cases | No |
| 12. HLA-linkage | Yes (DR3, DR4) | No |
| 13. Pathogenesis | Absolute insulin deficiency | Insulin resistance with relative insulin deficiency |
| 14. Serum C-peptide level | Very low to absent | Normal or high |
| 15. Predisposing factors | Viral infections, toxins | Obesity, lack of physical activity |
| 16. Insulin requirement for treatment | Always | In some situations |
Other Specific Types
There are several forms of DM associated with underlying conditions:
Genetic defects of β cell function: In these disorders, insulin secretion from β cells is impaired. These are called as maturity-onset diabetes of the young (MODY). They are inherited in an autosomal dominant manner and they are caused by mutations in genetic loci such as hepatic nuclear factor, glucokinase, etc.
Genetic defects in insulin action: These result from mutations in insulin receptor gene.
Diseases of exocrine pancreas: Diseases causing generalized pancreatic damage can result in DM. These include cystic fibrosis, hemochromatosis, chronic pancreatitis, trauma, pancreatectomy, and pancreatic cancer.
Endocrine disorders: Several hormones inhibit the action of insulin. Excessive secretion of these hormones will cause DM. Hyperglycemia is corrected following resolution of the primary endocrinopathy. Endocrine disorders associated with hyperglycemia are:
- Acromegaly: Excess growth hormone.
- Cushing’s syndrome: Excess cortisol.
- Glucagonoma: Excess glucagon
- Pheochromocytoma: Excess epinephrine.
- Hyperthyroidism: Excess thyroxine
Drug- or chemical-induced DM: Drugs or chemicals can impair insulin secretion or insulin action. Destruction of β cells and formation of islet cell antibodies have also been reported with some drugs. Examples include thiazide diuretics, α-interferon, and glucocorticoids.
Infections: Certain viral infections (such as Coxsackie virus B, congenital rubella, cytomegalovirus) can cause destruction of β cells.
Other genetic syndromes sometimes associated with DM: Many genetic syndromes (e.g. Down’s syndrome, Klinefelter’s syndrome, Turner’s syndrome) are associated with increased risk of developing DM.
Gestational Diabetes Mellitus (GDM)
This refers to the onset or first recognition of glucose intolerance during pregnancy. GDM occurs in 2-3% of all pregnant women. It is associated with increased risk of high birth weight of the newborn, cardiac defects, polyhydramnios, intrauterine fetal loss (due to placental insufficiency), premature birth, hypertension during pregnancy, pre-eclampsia, and alteration in duration of pregnancy. Early diagnosis and treatment of GDM are essential to prevent perinatal morbidity and mortality. After delivery, GDM can have following course:
- Return to normal glucose tolerance (however, many of these patients are likely to develop DM during subsequent years), or
- Persistence of DM or impaired glucose tolerance.
Patient should be reassessed 6 weeks or later following delivery.
Risk factors for GDM are given below:
- Past history of GDM
- Previous high-birth-weight baby
- Obesity
- Family history of diabetes mellitus
- High-risk ethnic group: South Asian or African.
- Comment
- Posted by Dayyal Dg.