Biochemical Cardiac Marker Studies

Myocardial cell necrosis leads to membrane damage and leakage of cell contents into the bloodstream. This forms the basis for the measurement of biochemical markers of myocardial injury in blood.
Various biochemical markers for myocardial injury are listed in Table 1202.1.
Previously, total creatine kinase, LD, and AST were used for the diagnosis of MI. However, due to their low specificity and due to the availability of more specific markers, these enzymes are now rarely measured. Currently, myoglobin (an early marker) and cardiac troponin (a definitive marker) are the recommended markers for diagnosis of MI; if cardiac troponin is not available, CK-MB (mass assay) is the next best alternative.
Usefulness of cardiac markers depends on the time of specimen collection after myocardial infarction. Use of the combination of markers and serial changes are more helpful (Table 1202.2).
An ideal cardiac marker should be highly sensitive, highly specific, should help to improve patient outcome, and be cost-effective. Such a marker is currently unavailable.
Role of biochemical cardiac markers in acute coronary syndrome:
- To confirm or exclude the diagnosis of acute myocardial infarction in cases with sudden onset of chest pain: In the presence of typical history and ECG findings consistent with acute MI, measurement of biochemical markers does not provide additional information for initial management. These patients need urgent treatment in the form of thrombolytic therapy or angioplasty or both. If the diagnosis is uncertain from clinical features and ECG in an emergency setting, biochemical markers are helpful in ruling out myocardial infarction.
Serial determinations (at admission, 6-9 hours, and 12-24 hours) are recommended to rule in or rule out the diagnosis of acute myocardial infarction. Use of CK-MB (mass) and cardiac troponin is recommended for diagnosis.
- Detection of old (by some days) myocardial infarction by cardiac troponin
- Diagnosis of reinfarction (CK-MB mass assay)
- To assess effectiveness of immediate reperfusion therapy (thrombolysis or percutaneous coronary intervention) in STEMI.
- Risk stratification to determine the likelihood of acute coronary syndrome
Creatine kinase: Highest activity of CK is present in striated muscle, brain, and heart.
Causes of increased CK are as follows:
- Disorders of skeletal muscle: Trauma, intramuscular injection, vigorous exercise, dermatomyositis, muscular dystrophy
- Disorders of heart: Myocardial infarction, myocarditis
- Disorders of the central nervous system: Cerebrovascular accident, head injury, generalized convulsions
- Disorders of the thyroid: Hypothyroidism
CK-BB, CK-MB, and CK-MM are the isoenzymes of CK. CK-BB predominates in brain, CK-MB in cardiac muscle, while CK-MM in skeletal muscle and heart. CKMB is the most cardiac-specific CK isoenzyme, and it is recommended to measure CK-MB mass.
Total serum CK and CK-MB are always elevated following MI. However, serum CK and CK-MB can arise from tissues other than heart. Following MI, CK-MB rises within 3-6 hours after the onset of symptoms, peaks within 12-24 hours, and returns to normal level by 48-72 hours.
*Currently recommended markers
|
| Markers | Time for detection | Peak | Return to normal |
| Myoglobin | 1-3 hr | 6-9 hr | 1day |
| CK-MB | 3-6 hr | 12-24 hr | 2-3 days |
| Troponin | 4-8 hr | 12-24 hr | 5-10 days |
Relative index or RI ([CK-MB/total CK × 100) is used to distinguish cardiac from skeletal muscle damage; RI above 5% is highly suggestive of acute myocardial infarction.
It is recommended to obtain sequential samples (one at presentation and subsequently at 8-hour intervals for 24 hours).
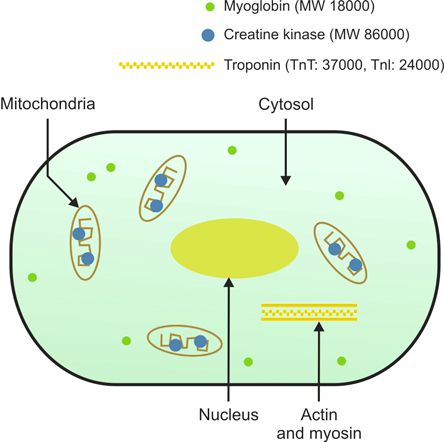
Myoglobin: Myoglobin is the oxygen-binding low molecular weight protein of cardiac and skeletal muscle cells. Myoglobin rises early after MI (1-3 hours) and is currently the earliest marker. Myoglobin of cardiac muscle cannot be distinguished from that of skeletal muscle. Myoglobin levels are raised following MI, open heart surgery, muscle injury, muscle dystrophy, renal failure, shock, and trauma. Thus, although myoglobin rises early following MI, it is not cardiac-specific.
However, non-elevation of myoglobin (in two sequential samples 2-4 hours apart) is helpful for exclusion of early MI in patients presenting with chest pain at emergency department.
Troponins (Tn): Cardiac troponin T (cTnT) and cardiac troponin I (cTnI) are the most sensitive and specific of the available markers of myocardial necrosis and are considered ideal markers for definitive diagnosis (either cTnT or cTnI). Troponins regulate the interaction of actin and myosin filaments during myocardial contraction.
Following MI, troponins appear in blood at about the same time as CK-MB. If troponins are elevated at least 12 or more hours following onset of chest pain, their diagnostic sensitivity is 100%. TnI is more cardio-specific as it is found only in heart muscle. It is not elevated following skeletal muscle injury. Following myocardial damage, TnI rises 4-8 hours the onset of chest pain, peaks within 12-24 hours, and remains elevated for 7-10 days. Development of assays for TnI and TnT represent a major advance in the diagnosis of MI. As troponins remain elevated for 7-10 days, they are useful in cases presenting late. If the onset of chest pain is 9-12 hours before admission, only troponin needs to be measured.
REFERENCE RANGES
- Lipid profile:
– Serum cholesterol: Desirable level: <200 mg/dl
– Serum triglycerides: Desirable level: <150 mg/dl
– HDL cholesterol: >60 mg/dl
– LDL cholesterol: <130 mg/dl
– LDL/HDL ratio: 0.5-3.0 - Biochemical cardiac markers:
– CK-MB: <5% or <10 μg/L
– Cardiac Troponin T: <0.1 μg/L
– Myoglobin: < 90 μg/L
CRITICAL VALUES
- CK-MB: >5% or >10 μg/L
- Cardiac Troponin T: >0.1 μg/L
- Myoglobin: >110 μg/L
References
- Achar SA, Kundu S, NorcrossWA. Diagnosis of acute coronary syndrome. Am Fam Physician 2005;72: 119-26.
- Bock JL. Test strategies for the detection of myocardial damage. Clin Lab Med 2002;22:357-75.
- Crook MA. Clinical chemistry and metabolic medicine 7th Ed. London. Edward Arnold (Publishers) Ltd. 2006.
- Eaton CB. Hyperlipidemia. Prim Care Clin Office Pract 2005;32:1027-55.
- Executive Summary of The Third Report of The National Cholesterol Education Program (NCEP). Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III). JAMA 2001;285:2486-97.
- Koolman J, Roehm KH. Color Atlas of Biochemistry, 2nd Ed. Stuttgart. Thieme 2005.
- McDermott MT. Endocrine secrets. 4th Ed. Philadelphia: Mosby, 2005.
- Senger AK, Jaffe AS. The use of biomarkers for the evaluation and treatment of patients with acute coronary syndromes. Med Clin N Am 2007;91:657-81.
- The Joint European Society of Cardiology/American College of Cardiology Committee: Myocardial infarction redefined-A consensus document of The Joint European Society of Cardiology/American College of Cardiology Committee for the redefinition of myocardial infarction. Eur Heart J 2000;21:1502-13.
- Tiyyagura SR, Smith DA. Standard lipid profile. Clin Lab Med 2006;26:707-32.
- Read Comments
- Posted by Dayyal Dg.